An ever-growing number of medical procedures exists in the healthcare profession. These can be anything from the most complex surgeries to everyday procedures, and perhaps one of the most common is the process known as venepuncture. This article outlines what happens during the typical venepuncture procedure.
What is venepuncture?
Venepuncture might sound scary; it's multi-syllabic, it has ‘puncture’ in it, and it sounds technical. In reality, venepuncture is just medical-speak for putting a hole in the vein to gain access to it. It entails passing a hollow needle into a superficial (surface level) vein. It is a procedure that takes place millions of times daily over the world, and has relatively few complications, causes relatively little pain, and takes relatively little time.
Venepuncture is normally performed for one of two reasons. The first of these is phlebotomy or the drawing of blood. This will be done when doctors need a sample of your blood to perform one of a variety of tests when trying to diagnose health problems. The other is to enable the giving of intravenous injections. This could be done if a healthcare professional needs to inject medication (such as some vaccines) into the vein, or for such things as drips.
|
|
What are the steps of venepuncture?
The typical venepuncture can be divided into a four-phase procedure, each of which is discussed below:
Explanation and Consent
The first part of a venepuncture procedure is confirming the patient’s identity. After this, the reason for the procedure and what it entails for that patient is explained by the healthcare professional in charge of the venepuncture.
The few risks are explained, and any relevant medical history (such as what medication the patient may be using) is collected from the patient. The patient is then asked if they have a preference for where to make the insertion (if there is nothing medically restricting this), and they are asked for their consent to go ahead with the procedure.
.webp?width=795&name=Untitled%20design%20(73).webp)
Preparation
This phase entails preparing both the equipment being used and the patient. The equipment should have been properly sterilised before the procedure and allowed time to dry. Once this has happened, the equipment is gathered and brought to the patient, after the medical professional has thoroughly cleaned their hands.
The patient’s details should be reconfirmed (particularly if, for example, a doctor performed the Explanation and Consent phase and a nurse is performing the rest of the procedure), and following confirmation, an appropriate vein is selected and prepared. This is done by tapping it. If a vein is too hard, cord-like, intersects another vein, or does not respond to tapping, then another vein should be selected. A tourniquet is applied around four finger lengths above the vein, and the next phase begins.
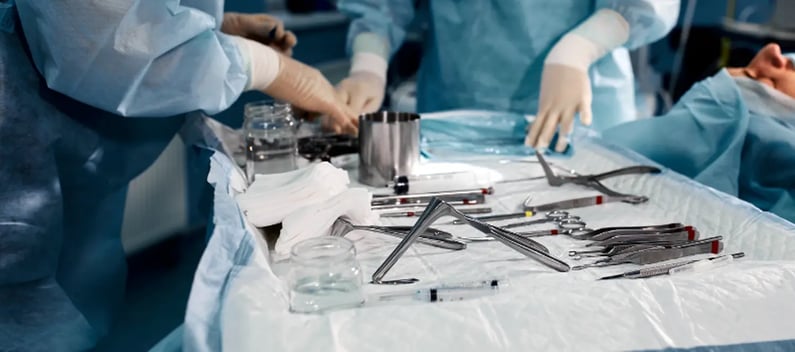
Make sure that all equipment is sterile before operating.
Procedure
The actual venepuncture follows, by the practitioner wearing the appropriate equipment (namely, gloves). The puncture site should be cleaned with disinfectant wipes, and allowed to air dry.
With a tourniquet applied, the needle is then inserted through the skin into the vein. If blood is being drawn, the appropriate containers are attached to the tubes.
After the blood is drawn, cotton wool is placed over the puncture site as the vein is retracted. The wool is applied with pressure for 60 seconds and then secured with tape. The needle is then disposed of. If the collection didn’t work properly, the procedure is repeated.
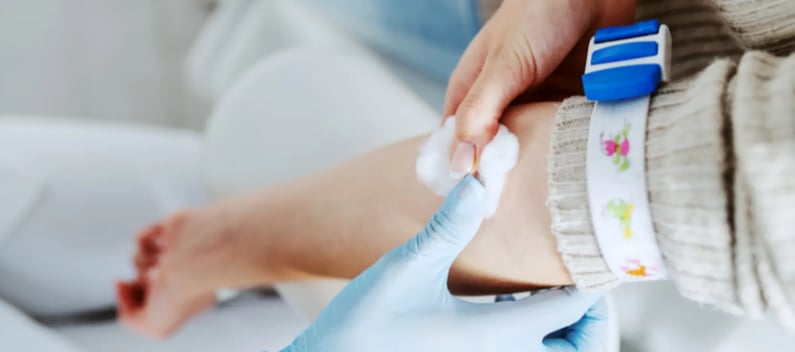
Apply pressure on the puncture site and then secure with tape.
Aftercare
Aftercare is the final stage of a venepuncture procedure. Aftercare entails making sure the patient gets the appropriate treatment for any complications that may arise after the procedure.
For venepuncture, the medical professional will tell a patient to get in contact with the nursing staff or their general practitioner if the puncture site becomes red, swollen, hot, or painful.

Specialist Care training teaches healthcare professionals more about specialist areas of health and social care in order for them to meet their CPD goals, including courses that focus on elements practised in venepuncture such as Sharps and Needles Awareness and Blood Transfusions.

-1.webp?width=243&height=74&name=Logo%20R%20Homepage%20White%20Final%20Horizontal%20Large%20NEW%20small%20(2)-1.webp)
.webp?quality=low&width=600&name=Flexebee%20Online%20Training%20Venepuncture%20(1).webp)

COMMENTS